The way women train is changing.
More women are training through pregnancy and wanting to return to the gym as soon as possible post natal.
Awareness is growing around the issues post natal women face and how this relates to their health and fitness goals.
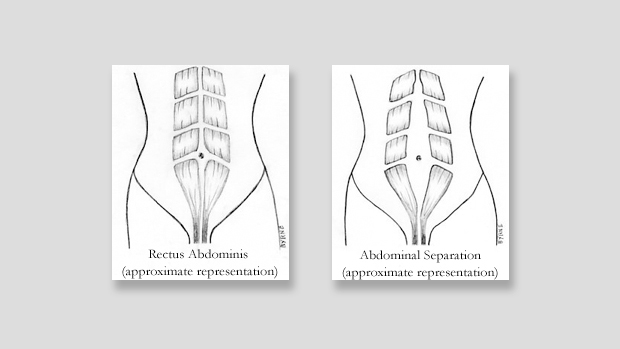
One of those areas is Diastasis Recti, otherwise known as Abdominal Separation.
Abdominal separation is something that, until recently, unless you worked in the post natal space or had personally been diagnosed with it most people had no idea what this was.
Worse still most Post Natal women didn’t even know they should to be checked for it.
In my last post we spoke about the anatomical side of abdominal separation.
In this post were going to cover a little more about what it means and why you should be concerned by it.
As a Post natal woman Ab sep is technically any separation 2 fingers or more.
You need to remember abdominal separation is very common and a 2 finger separation at birth is considered “normal”
It’s not only the width you should be concerned about but the depth and length also needs to be considered.
You might have a 2 finger separation that’s shallow and only around your belly button.
This shows the muscles below the separated rectus are of good quality and providing adequate support for the trunk.
You might have a 1.5 finger width separation but it’s very long and deep.
This would indicate the layers of muscles below aren’t providing the necessary support for your trunk as they too have been compromised by the separation.
Or you could have the triple effect of a wide, deep and long separation.
Like no two pregnancies are the same, the same goes with abdominal separation, every woman may experience the effects to a lesser or greater degree.
The main thing to remember is with the correct guidance it’s possible to regain full function of the abdominals and core strength, even if the gap does not fully repair.
Why is Abdominal Separation a concern?
And why do we need to look at the bigger picture when correcting it?
The key point is that an abdominal separation contributes to the instability and weakness of the core (which helps support the spine and maintains or contains natural internal pressure).
The muscles of your core can no longer fully support your pelvic and abdominal region and creates an inability of the transverse abdominis to effectively support the abdominal organs.
- Pelvic Floor Dysfunction
Diastasis recti and PF disfunction tend to go together. Studies have shown 66% of women who have Ab Sep have some level of PF disfunction (Spitznagle et al 2007)
- Prolapse or Hernia
Another effect of your core not doing its job correctly is excessive intra abdominal pressure going in the wrong direction, which would be outwards and downwards. Its this the same excessive, uncontainable pressure that can cause organ hernia or organ prolapse.
Organ hernia
is when your internal organ(s) protrude through the separation.
Organ prolapse
is when a pelvic organ-such as your bladder-drops (prolapses) from its normal place and pushes against the walls of your vagina.
Both an organ hernia and an organ prolapse has varying degrees of severity.
Abdominal Separation and lower back pain
As the abdominals provide support for your spine if the strength and support they provide has been compromised by Ab Sep it can lead to lower back pain.
It can also effect your posture – again leading to lower back pain.
No longer are “just dealing with it” or having surgery the only options women have when it comes of both PF disfunction and abdominal separation.
So what can you do?
If you are concerned you may have abdominal separation I would advise the following:-
- Have it correctly diagnosed by a health professional, preferably a women’s health specialist physio.
- Follow the advice and exercises prescribed to the letter
- Ensure the work you do alongside this complements the internal work prescribed by the physio, where possible seeking the advice of a specialist Pre and Post Natal Personal Trainer
Like anything prevention is better than cure so taking the right steps during pregnancy to minimise the potential of it developing is a good place to start.